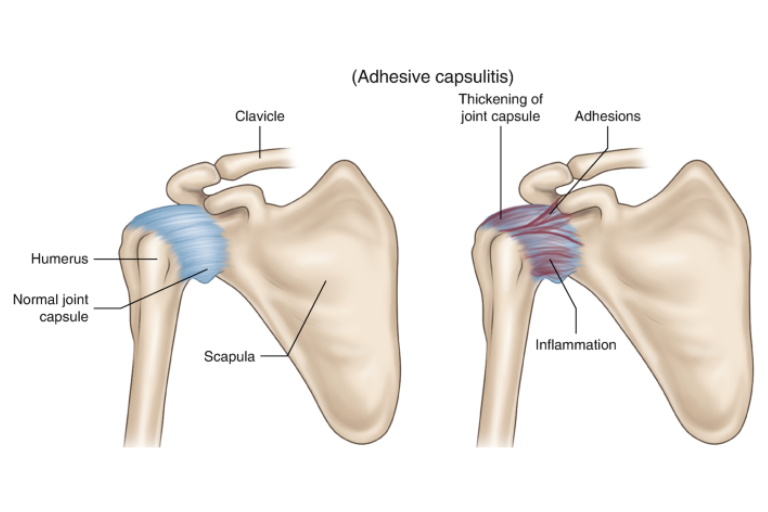
What is Frozen Shoulder?
Frozen Shoulder, medically known as Adhesive Capsulitis, is a painful and progressively stiffening condition of the shoulder joint.
It occurs when the capsule (a thin tissue covering the shoulder joint) becomes inflamed, thickened, and tight — leading to restricted motion in all directions.
Patients commonly describe a gradual onset of pain followed by difficulty in performing simple activities like combing hair, reaching overhead, or tucking in a shirt.
It’s often self-limiting, but recovery may take several months to years if left untreated.
⚙️ How Does it Develop?
The shoulder capsule normally allows smooth, fluid movement. In Frozen Shoulder, inflammation triggers the formation of scar tissue and adhesions, which make the capsule shrink and tighten around the joint.
This stiffness, coupled with pain, results in reduced movement — the “frozen” shoulder.
🧩 Stages of Frozen Shoulder & Their Duration
Stage 1: Freezing (Painful Stage)
🕐 Duration: 6 weeks – 4 months
- Persistent and worsening pain, even at rest or during sleep.
- Gradual stiffness sets in; range of motion starts decreasing.
- Inflammation is active during this stage.
🔹 Early diagnosis and treatment at this stage can shorten the overall disease course significantly.
Stage 2: Frozen (Stiffness Stage)
🕐 Duration: 4 – 8 months
- Pain may reduce slightly, but stiffness peaks.
- Daily activities like reaching behind the back or overhead become very difficult.
- The capsule remains thick and contracted.
🔹 Stretching and guided physiotherapy are most crucial in this phase.
Stage 3: Thawing (Recovery Stage)
🕐 Duration: 6 months – 1 year
- Pain subsides gradually.
- Shoulder motion slowly improves as adhesions release.
🔹 With consistent rehabilitation, most patients regain near-normal shoulder function.
⚠️ Risk Factors
- Age 40–65 years
- More common in women and diabetics
- Thyroid disorders (hypo/hyperthyroidism)
- Prolonged shoulder immobilization (after injury or surgery)
- Cervical spine disorders
- Post-cardiac or breast surgery
- History of previous shoulder surgery or trauma
🔬 Etiology & Pathophysiology
Frozen Shoulder can be:
- Primary (Idiopathic): develops spontaneously without clear cause, often linked with metabolic or autoimmune factors.
- Secondary: follows trauma, surgery, or prolonged immobility.
Pathologically, the shoulder capsule and synovium become inflamed (synovitis) → leading to fibrosis and contracture → resulting in capsular thickening, especially around the rotator interval and coracohumeral ligament.
🧪 Investigations
- Clinical Examination:
- Global restriction of active and passive movement (especially external rotation).
- Painful end-range in all directions.
- Imaging:
- X-ray: Usually normal; rules out arthritis or calcific tendinitis.
- MRI Shoulder: May show capsular thickening and reduced joint volume, helping to confirm diagnosis and rule out rotator cuff tears.
💊 Management
🩹 Non-Surgical (Mainstay)
- Pain control: Anti-inflammatory medication and ice/heat therapy.
- Ultrasound-Guided Injections:
- Corticosteroid injections in early (freezing) stage to reduce inflammation.
- Hydrodilatation (joint capsule distension with saline + steroid) to stretch the capsule.
- Physiotherapy:
- Early supervised passive mobilization, pendulum and stretching exercises.
- Gradual strengthening once pain subsides.
- Home Exercise Protocol:
- Regular movement is key — “move it or lose it” principle.
🩺 Surgical (For Resistant Cases)
- Arthroscopic Capsular Release:
- Keyhole surgery to cut tight bands of the capsule and immediately restore motion.
- Followed by early, aggressive physiotherapy for sustained results.
⏳ Importance of Early Diagnosis
Early identification during the freezing stage is crucial.
Prompt anti-inflammatory and physiotherapy-based management can prevent capsular fibrosis, shorten recovery time, and help avoid surgery.
Delayed diagnosis, on the other hand, prolongs stiffness and increases the risk of chronic limitation of shoulder movement.
🌟 Prognosis
With appropriate, stage-specific treatment, 90–95% of patients achieve excellent recovery.
In diabetics or neglected cases, recovery may be slower, but outcomes remain good with consistent therapy.
💬 Key Takeaway
“Frozen Shoulder doesn’t mean your shoulder will stay frozen forever — with early intervention and guided physiotherapy, movement and comfort can be completely restored.”